Welcome to our blog! We periodically update our blog with questions from our patients, important issues or trends in dental care, and other important information for our patients in Mesa, Arizona.
North Stapley Dental Care’s blog will help you understand what to expect with Root Canal treatment, tooth extractions, keeping up with your dental care when traveling, bone grafting, and help with understanding dental needs for your children.
If you have any other questions, or have a topic you’d like to see us cover, please reach out to us and let us know!
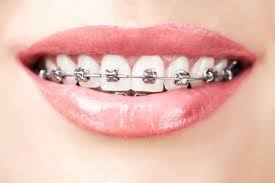
How Braces Affect Tooth Health
Traditional metal braces have been used to straighten countless teeth resulting in countless beautiful smiles. However, there is a downside to braces that many don’t
The Future of Dentistry
The practice of dentistry has existed since 7000 BC, and yet it continues to evolve. Due to new technology and techniques, dentistry is a changing

What Type of Toothpaste Do I Need?
Dental plaque is a biofilm of bacteria and sugar that constantly forms on our teeth. The problem with dental plaque is that it is acidic

What is a Root Canal
Needing a root canal can sound scary for many. The root canal procedure is often misunderstood. While is the procedure can be complex and fairly

Tooth Decay Facts
What do you really know about tooth decay? Is it inevitable? Is sugar really bad? We’ve compiled 7 facts you should know to better protect

Pregnancy and Dental Care
Pregnant women have a unique set of circumstances that affect their teeth, however, having dental check-ups and cleanings is safe and important during pregnancy. Dental

Causes and Remedies for Tooth Sensitivity
Tooth sensitivity can be a debilitating problem for many patients. When patients come to our office with tooth sensitivity pain – we start by asking

Cosmetic Dentistry: What Are the Best Options
Adults sometimes find that their smiles are lacking something they would like to see when they look in the mirror. If this is the case

Teens and Dental Care
Empowering Teens to Take Control of their Oral Health Teenagers in general have notoriously bad dental habits. It is not uncommon for us to see

Proper Dental Care when Traveling
Ensuring proper care of your teeth while on the road. Whether it is vacation travel or business travel, regular and thorough dental care sometimes loses

Does Your Child Grind His or Her Teeth at Night?
Bruxism, or the grinding of teeth, is remarkably common in children and adults. For some children, this tooth grinding is limited to daytime hours, but

Your Child’s Diet and Their Oral Health
A child’s general level of health often dictates his or her oral health, and vice versa. Therefore, supplying children with a well-balanced diet is more

Help Prevent Cavities with Fluoride
Fluorine has proven to be effective in minimizing childhood cavities and tooth decay. Fluoride is a key ingredient in many popular brands of toothpaste, oral
Homecare After Tooth Extractions
While a tooth extraction can be a serious dental procedure, aftercare is just as critical as the procedure itself. As the dental patient, it is

Root Canal Therapy
Root canal therapy is needed when the nerve of a tooth is affected by decay or infection. In order to save the tooth, the pulp

Cracked Tooth
Cracked and fractured teeth are common dental problems. As people retain their natural teeth longer (due to advances in dental technology), the likelihood of cracked

After Dental Implant Surgery
Home Care for Dental Implants Following dental implant surgery, patients must take detailed care of the area surrounding their new implant. For the first month

Tooth Extractions
Tooth Extractions and Oral Surgery in Mesa If you are experiencing extreme sensitivity or are suffering from advanced periodontal disease, you may be required to

Bone Grafting
Bone grafting is often closely associated with dental restorations such as bridge work and dental implants. In the majority of cases, the success of a

Why Are Primary Teeth Important
Primary teeth, also known as “baby teeth” or “deciduous teeth,” begin to develop beneath the gums during the second trimester of pregnancy. Teeth begin to

When Will My Baby Start Getting Teeth?
The initial growth period for primary (baby) teeth begins in the second trimester of pregnancy (around 16-20 weeks). During this time, it is especially important

How to Prevent Cavities
Childhood cavities, also known as childhood tooth decay and childhood caries, are common in children all over the world. There are two main causes of
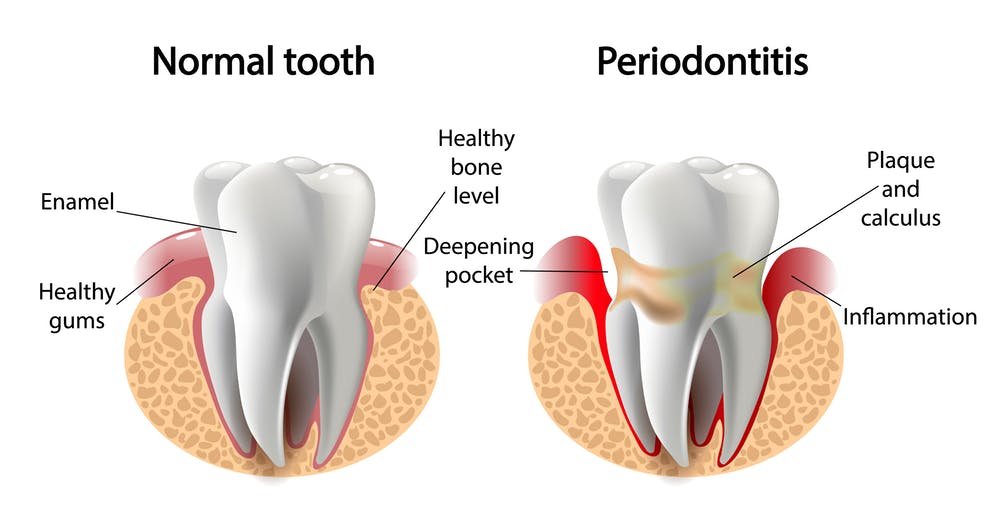
Periodontal Disease
What Is Periodontal Disease? The word periodontal means “around the tooth”. Periodontal disease attacks the gums and the bone that support the teeth. Plaque is a sticky
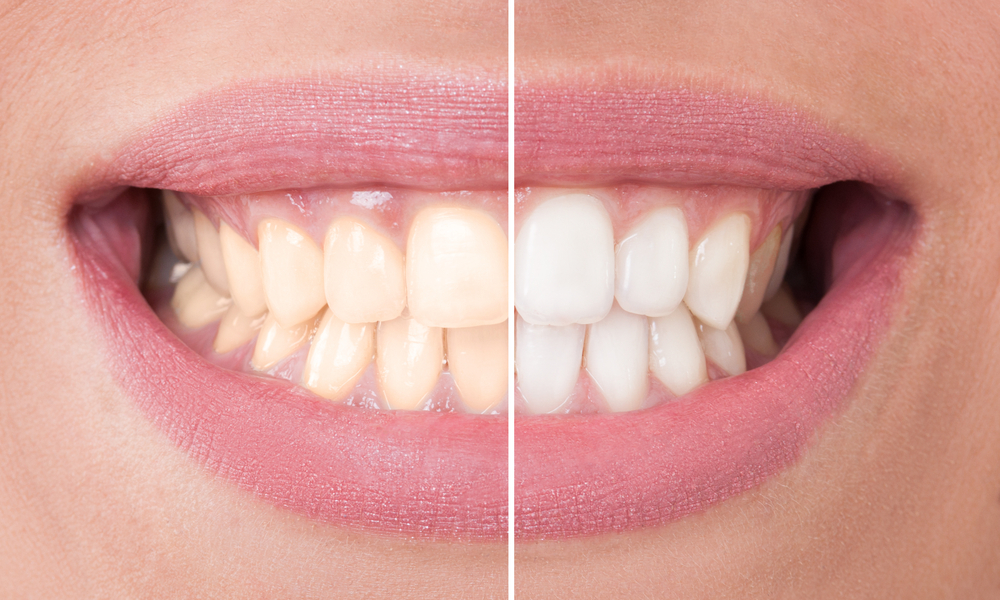
Teeth Whitening
Like many of our patients, your teeth aren’t as white as you’d like, and you may feel unhappy with the color of your teeth. Fortunately,
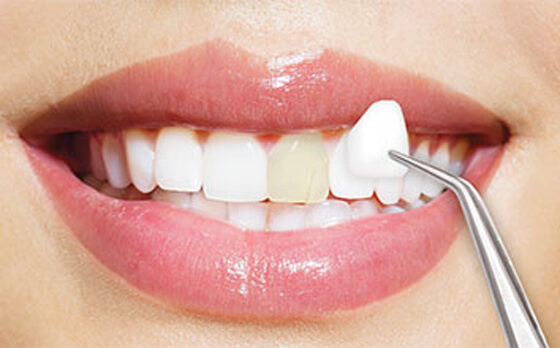
Porcelain Veneers
What Are Dental Veneers? Veneers are very thin pieces of durable, tooth-shaped porcelain custom made to go over your tooth (for shape and color). Veneers

